Winner of Access to Understanding 2013
X-rays can now be used not only to show where bones have fractured, but
also to investigate why these bones break in the first place. Results suggest
the possibility of preventing the trauma of thousands of broken hips using
drugs already commonly used for treating osteoporosis.
Normal healthy bones can be thought of as nature’s scaffold poles. The
tightly packed minerals which make up the cortical bone form a sheath around an
inner core of spongy bone and provide the strength which supports our bodies.
Throughout our lives, our skeletons are kept strong by the continuous creation
of new, fresh bone and the destruction of old, worn out bone. Unfortunately, as
we age destruction becomes faster than creation, and so the cortical layer
thins, causing the bone to weaken and break more easily. In severe cases, this
is known as osteoporosis. As a result, simple trips or falls which only bruise
a younger patient can cause serious fractures in the elderly. However, half of
elderly patients admitted to hospital with a broken hip do not suffer from
osteoporosis.
hip fractures are debilitating. Repairing one requires traumatic surgery that,
even if successful, may not enable a patient to regain the full mobility they
had beforehand. The National Osteoporosis Society estimates that 13,800 people
in the UK die every year as a direct result of hip fractures. This is over 10%
of patients injured. (http://www.nhs.uk/conditions/hip-fracture/Pages/introduction.aspx)
Therefore, understanding how these fractures occur and acting to prevent them
is vital for improving the quality and length of life of our aging population.
To better understand why hips fracture, researchers in Cambridge and
Prague analysed CT scans performed on the opposite, unbroken hips of a group of
elderly women admitted to Bulovka University Hospital, Prague with hip
fractures. Previous studies have shown that these tend to be in a similar
condition to the broken hip pre-fracture.
CT scanners are now standard pieces of equipment in most hospitals, and
are used to examine organs and tissues inside the body. Essentially a rotating
X-ray machine, a CT scanner takes many X-ray snapshots at different angles
around a body part to produce a 3D image of its internal structure. X-rays are
energetic waves of energy which are partially absorbed by the materials they
pass through. The amount of absorption depends on the density of the structure
encountered – denser structures, like bone, absorb more of the X-ray energy,
leaving less energy to be measured by the detector on the other side. However,
the resolution of the images collected by a standard hospital CT scanner is not
sensitive enough to accurately determine the thickness of the cortical bone.
researchers in Prague and Cambridge were able to extract information from
clinical CT scans that was sensitive enough to produce coloured maps on the
surface of a model hip showing the variation of cortical bone thickness in more
detail than ever. Variations in thickness of only 30 microns – the size of a
grain of dust – could be detected.
The results were striking. Not only did the women with fractured hips
have generally thinner cortical bone than normal, but some patients also had
local patches of even thinner bone. This was the case even in women who did not
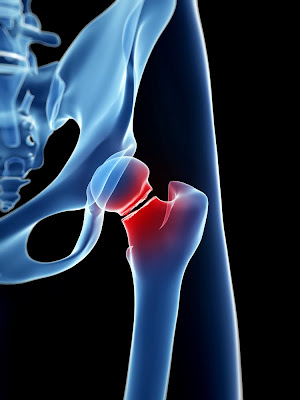
suffer from osteoporosis. Most importantly, the extra-thin regions were found
on the femoral neck – the part of the hip bone where fractures most commonly
occur. In some patients, these patches were 30% thinner than the surrounding
bone, and as big as a thumbnail. These weaker points provide the ideal conditions
for a crack to form and subsequently grow into a fracture. Further studies are
needed to confirm whether these localised regions do act as the starting point
for a fracture, but at the very least they affect the type, and hence severity,
of fracture which occurs. They could also explain the mystery of spontaneous
hip fracture, which accounts for 6% of hip fractures – 4000 broken hips a year
in the UK, which break for no known reason.
The research team have named these local patches of thinner bone ‘focal
osteoporosis’. However, despite the name it is not yet known if these areas can
be strengthened using standard osteoporosis drugs, which slow down the natural
destruction of bone cells. An extensive clinical trial will be needed to
investigate further, but if the focal patches do respond to treatment it raises
the tantalising possibility of a future where many fractures could be treated
before they even form. The improvement this would have on our quality of life
in our old age would be invaluable.
This entry
Cortical thickness mapping to identify focal osteoporosis in patients with hip fracture
PMCID: PMC3372523
Kenneth E. S. Poole, Graham M. Treece, Paul M. Mayhew, Jan Vaculík,
Pavel Dungl, Martin Horák, Jan J. Štěpán, and Andrew H. Gee
PLoS One (2012) 7(6), e38466
Access to Understanding entrants are asked to write a plain English summary of a research article. For Access to Understanding 2013 there were 9 articles to choose from, selected by the Europe PMC funders.
The articles are all available from Europe PMC, are free to read and download, and were supported by one or more of the Europe PMC funders.
Look out here and on Twitter @EuropePMC_news for announcements about the competition.





What a well written summary! No wonder it won the competition. I had not heard of focal osteoporosis before. It will be interesting to find out if the focal patches respond to treatment.
Very nice article! Do you know if a clinical trial is in the works? This would be of particular interest for those dealing with Transient Migratory Osteoporosis. TMO generally resolves on its own, but is extremely painful, with substantial disability due to the restriction of all weight bearing activity for the couse of the disorder.
Do we know why AVN can be associated with this & what the treatment option would be?
What a well written summary! No wonder it won the competition. I had not heard of focal osteoporosis before. It will be interesting to find out if the focal patches respond to treatment.